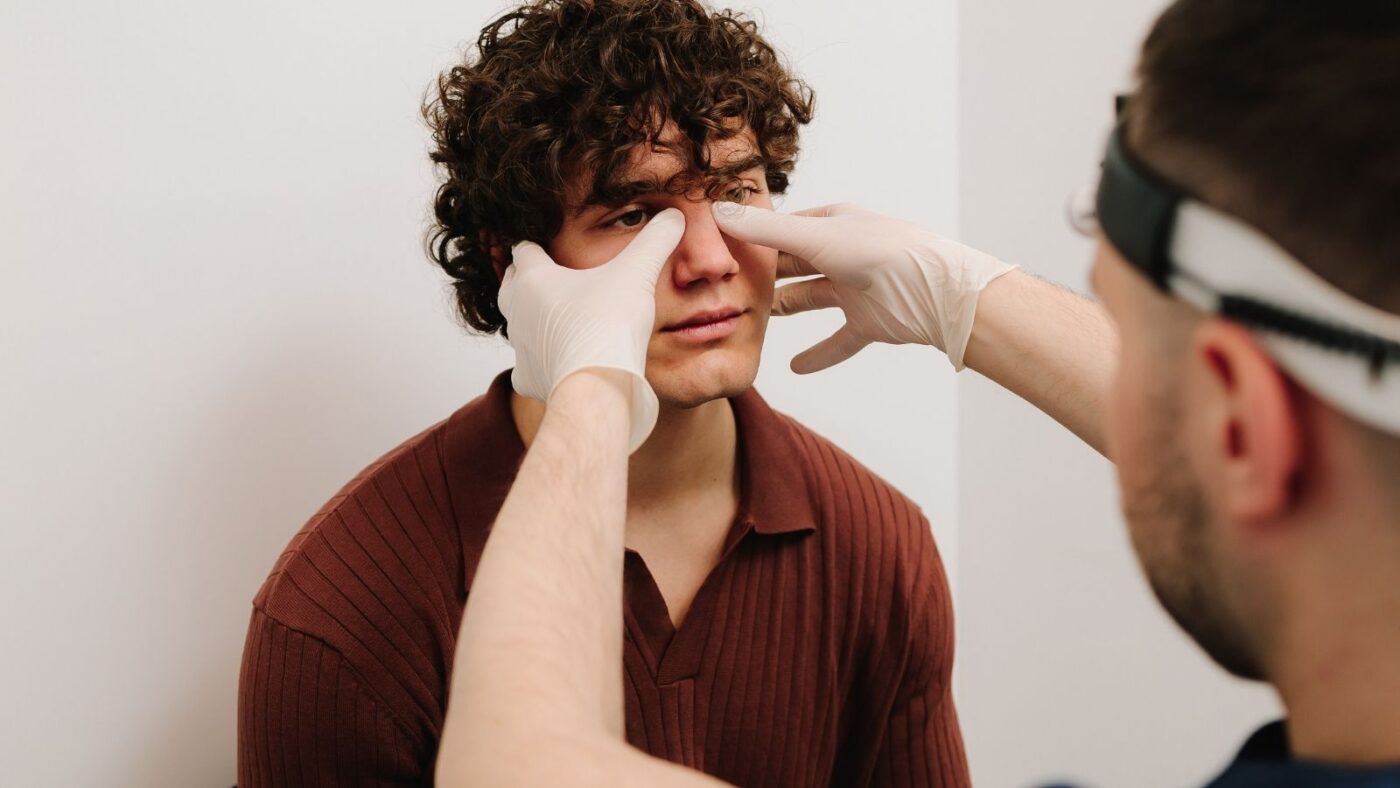
Nasal fracture is the most common type of fracture we encounter in the facial region and is referred to in medical literature as a “nasal fracture.” It is the condition in which the integrity of the nasal bones and cartilage structures that form our nose is disrupted as a result of an external impact. Consider that our nose, positioned right in the center of our face and almost protruding outward, is naturally a target for trauma due to its location.
The nasal fractures of patients who apply to our clinic may present across a wide spectrum, ranging from a simple crack to complex comminuted fractures. The type and severity of the fracture vary depending on the direction and intensity of the impact and the individual’s nasal anatomy. In some of our patients, only the nasal bones are affected, while in those who have experienced more severe trauma, the cartilage structures inside the nose, the septum (the wall in the middle part of the nose), and even the surrounding facial bones may also be damaged.
İçindekiler
Types of Nasal Fractures
We classify nasal fractures in various ways according to the structures affected and the characteristic features of the fracture:
- Simple Fractures: Fractures in which only the nasal bones are affected, there is no open wound on the skin, and there is no significant distortion in the shape of the nose. They usually occur as a result of mild trauma and are relatively easy to treat. For example, they may develop after a light impact from a ball while playing basketball.
- Complicated Fractures: Fractures in which, in addition to the nasal bones, the septum, cartilage structures, or surrounding bones are also affected. In these types of fractures, noticeable distortion in the shape of the nose, difficulty breathing, and other complications are observed. We encounter these types of fractures more frequently in high-energy traumas such as traffic accidents.
- Open Fractures: Fractures in which the fracture line opens to the surface of the skin, meaning there is a wound or cut on the skin. They require urgent intervention due to the risk of infection. In such fractures, cleaning the wound and appropriate antibiotic treatment are of vital importance.
- Closed Fractures: Fractures in which there is no open wound on the skin and the fracture line remains beneath the skin. In practice, the vast majority of nasal fractures are of this type and generally carry a lower risk of complications.
- Displaced Fractures: Fractures in which the fracture fragments have shifted from their normal anatomical positions. They cause noticeable distortion in the shape of the nose and usually require surgical intervention. Patients often present with the complaint, “My nose is crooked,” when they look in the mirror.
- Non-displaced Fractures: Fractures in which the fracture fragments remain in place and there is no noticeable change in the shape of the nose. Although these patients may experience pain and tenderness, there is generally no aesthetic problem.
In our clinical practice, nasal fractures account for approximately 40–50% of all facial fractures. One out of every two patients presenting to emergency departments due to facial trauma is found to have a nasal fracture. This high rate is directly related to the position of the nose on the face and its protruding structure.
Although nasal fractures can be seen in all age groups, we observe a marked increase in frequency among young men aged 15–30. This is associated with factors such as greater participation in physical activities and contact sports, more frequent exposure to traffic accidents, and unfortunately, greater involvement in incidents of physical violence. In women, nasal fractures resulting from falls and household accidents are more commonly encountered.
Causes and Mechanisms of Nasal Fractures
Nasal fractures occur as a result of direct or indirect trauma to the nose. The severity, direction, and type of trauma determine the type and seriousness of the fracture. The anatomical structure of the nose and the individual’s age also play an important role in the formation of fractures. For example, in elderly patients, even milder trauma can cause fractures due to the more fragile bone structure.
Most Common Causes
- Sports Injuries: Approximately one-third of nasal fracture cases presenting to our clinic occur during sports activities. Impacts occurring during contact sports (boxing, wrestling, rugby) and team sports (football, basketball, hockey) constitute a significant portion of nasal fractures. Situations such as being hit by a ball, receiving an elbow strike, or colliding with an opponent are common causes. The occurrence of a nasal fracture when two players jump for a header during a football match and one receives an elbow strike is a situation we frequently encounter in practice.
- Falls: Falls occurring inside or outside the home may lead to nasal fractures, especially in the elderly and children. Falling face down or slipping on stairs poses a risk. As in the case of one of our patients who slipped on icy ground, sudden and unexpected falls resulting in the face striking a hard surface are among the common causes of nasal fractures.
- Traffic Accidents: In-vehicle accidents involving impact with the steering wheel or dashboard, or facial trauma in motorcycle accidents when a helmet is not worn, may cause nasal fractures. Although the frequency of such injuries has decreased with the widespread use of seat belts, they still remain an important cause.
- Physical Violence: Punches or blows with hard objects are among the significant causes of nasal fractures. Nasal fractures related to violent incidents are more frequently seen, especially in individuals under the influence of alcohol.
- Work Accidents: In industrial fields such as construction and factories, nasal fractures may occur due to falling objects or contact with machinery. The risk increases further in work environments where protective equipment is insufficient.
Mechanisms of Fracture Formation
The mechanism of nasal fracture formation varies according to the direction and intensity of the impact. Understanding these mechanisms helps us both in diagnosis and treatment planning:
- Frontal Impacts: Direct blows to the front of the nose generally cause fractures in the middle of the nasal bones and collapse of the nasal dorsum. Septal injury is also common in these types of fractures. For example, a direct punch to the face may lead to a midline fracture of the nasal bone and inward collapse.
- Lateral Impacts: Lateral (side) impacts result in collapse on the side of the impact and deviation toward the opposite side. This may lead to a “C” or “S” shaped nasal deformity. In a patient who sustained this type of fracture after being struck on the side of the face by an opponent’s elbow while playing basketball, we observed that the nose had shifted noticeably to the right.
- Upward Impacts from Below: Blows coming from below may cause the nasal tip to lift upward and the septum to be pushed upward in a telescopic manner. These types of injuries are generally more complex and may lead to severe septal damage. For example, during a fall, if the chin hits the ground first and the impact energy is transmitted upward, this mechanism may be triggered.
- High-Energy Trauma: In very severe impacts, not only the nasal bones but also the surrounding facial bones (maxilla, ethmoid, frontal bones) may be affected. In such cases, “naso-ethmoidal” or “naso-orbital” fractures may occur. We encounter these types of complex fractures more frequently in traffic accidents or falls from height, and their treatment is also more complicated.
Risk Factors
Based on our clinical experience, we can say that certain conditions significantly increase the risk of nasal fractures:
- Engaging in contact sports: The risk is particularly high in sports such as boxing, wrestling, and rugby.
- Not using protective equipment: Not wearing helmets, face guards, or nasal protectors increases the risk.
- Balance problems or diseases with a high risk of falling: In conditions such as epilepsy, vertigo, and Parkinson’s disease, the risk of falling and thus nasal fracture increases.
- Alcohol or substance use: Increases both the risk of falling and the likelihood of involvement in violent incidents.
- Being in a violent environment: Being in situations involving domestic violence or fights increases the risk.
- Work environments with insufficient safety measures: The risk is particularly high among those working in construction and heavy industry sectors.
To prevent nasal fractures, it is important to use protective equipment during risky activities, take safety precautions, and act carefully. Simple measures such as using nasal protectors during sports and wearing seat belts while driving can significantly reduce the risk of nasal fractures. As I always tell my patients, adopting the principle of “prevention before treatment” is the most effective approach in preventing such injuries.
Symptoms Requiring Medical Intervention in Nasal Fractures
In cases of suspected nasal fracture, certain symptoms require urgent medical evaluation. Not every nasal trauma results in a fracture, but specific findings may indicate a serious injury and require rapid intervention. In my clinical practice, I frequently hear patients ask, “Should I see a doctor in this situation?” Here are the critical symptoms that answer that question:
Situations Requiring Emergency Intervention
- Uncontrolled Nosebleed: Bleeding lasting longer than 20–30 minutes after trauma and not stopping with pressure may indicate vascular injury. One of our patients presented to the emergency department with a nosebleed that had not stopped for 45 minutes after being struck during a basketball game. On examination, a bleeding vessel inside the nose required cauterization. Such bleeding may lead to blood loss and even shock.
- Clear Fluid Discharge: Clear, watery discharge from the nose or ear may indicate cerebrospinal fluid (CSF) leakage. This may be a sign of a skull base fracture and is very serious. Patients with CSF leakage are at risk of meningitis and require urgent neurosurgical consultation. A characteristic feature of this discharge is that when dropped onto a tissue, it forms blood in the center and a clear ring around it (halo sign).
- Severe Headache and Altered Consciousness: Severe headache, dizziness, nausea-vomiting, confusion, or fainting accompanying nasal trauma suggest the possibility of brain injury. In one of our patients who had a nasal fracture and mild confusion after a motorcycle accident, a small hemorrhage was detected on brain tomography. Such symptoms should never be ignored.
- Vision Problems: Double vision, blurred vision, or vision loss may indicate involvement of the bones around the eye. Particularly in orbital floor fractures, the eye muscles may become trapped, leading to double vision. This condition requires urgent ophthalmologic evaluation.
- Septal Hematoma: Accumulation of blood (hematoma) on both sides of the septum inside the nose may impair the nutrition of the cartilage tissue and lead to permanent damage if not drained urgently. A septal hematoma appears on examination as a soft, purplish-red swelling on both sides of the septum. If treatment is delayed, the septal cartilage may become necrotic (die) and a “saddle nose” deformity may develop.
Symptoms Requiring Evaluation
- Nasal Deformity: Noticeable curvature, collapse, or asymmetry of the nose strongly suggests the presence of a fracture. Patients often present with complaints such as “My nose is crooked” or “My nose has collapsed inward.” However, edema (swelling) that develops immediately after trauma may mask the underlying deformity. Therefore, it may be necessary to wait for the edema to subside (usually 3–5 days) for a definitive evaluation.
- Difficulty Breathing: Unilateral or bilateral nasal obstruction may result from edema or septal deviation. A boxer patient of ours presented with breathing difficulty described as “It feels like one of my nostrils is completely blocked.” On examination, we detected a severe deviation of the septum to the right.
- Facial Edema and Bruising: Swelling and bruising around the nose and under the eyes (raccoon eye appearance) are common findings. Especially bruising under the eyes occurs as blood and fluid descend due to gravity and becomes more pronounced 24–48 hours after trauma. Although this appearance may be dramatic, it usually resolves on its own.
- Nasal Mobility: Abnormal movement or a crackling sound (crepitation) when the nose is lightly touched indicates the presence of a fracture. This crackling sensation felt when gently pressing on the nasal bone during examination results from fracture fragments rubbing against each other and is a pathognomonic finding (i.e., definitively diagnostic).
- Pain and Tenderness: Throbbing pain that increases with touch is typical. Patients often describe it as “My nose is throbbing” or “Even wearing glasses causes pain.” This tenderness may persist until the fracture heals (usually 2–3 weeks).
Late Complication Symptoms
Symptoms that may appear days or weeks after trauma are also important and should not be neglected:
- Chronic nasal obstruction: May result from septal deviation or intranasal adhesions (synechiae).
- Recurrent nosebleeds: May develop due to mucosal damage or abnormal vascularization.
- Loss of smell: Should raise suspicion of skull base fracture or olfactory nerve damage.
- Chronic sinusitis findings: May occur due to impaired sinus drainage.
- Permanent change in nasal shape: Untreated fractures in a timely manner may result in permanent deformity.
One of our patients presented to our clinic with recurrent sinusitis attacks that did not respond to antibiotics after a nasal trauma he had experienced 6 months earlier. Evaluation revealed impaired sinus drainage due to the old fracture, and surgical intervention was required. This example is instructive in demonstrating the long-term effects of nasal fractures.
Diagnostic Process and Evaluation
The diagnosis of a nasal fracture requires a systematic evaluation process. This process includes a detailed medical history, physical examination, and imaging methods when necessary. In our clinic, this protocol applied to every patient forms the basis for accurate diagnosis and treatment planning.
Medical History and Initial Evaluation
As a physician, during my first encounter with the patient, I inquire in detail about how the trauma occurred. This information helps me estimate the possible type of fracture and associated injuries:
- Time and mechanism of trauma: The question “When and how did it happen?” is critical. For example, responses such as “3 hours ago, a ball hit me while playing basketball” or “I fell last night” are important for evaluating both treatment timing and expected findings.
- Direction and severity of the impact: The question “From where did the blow come?” helps us predict the type of fracture. Frontal impacts usually cause symmetrical collapse, while lateral impacts cause crookedness and deviation.
- Presence of loss of consciousness: The question “Did you faint during the incident?” is asked to assess the possibility of accompanying head trauma.
- Initial symptoms and their progression over time: Questions such as “What did you feel at first? How are you now?” are important for understanding the severity and progression of the condition.
- Previous nasal trauma or surgery: Previous trauma or surgical interventions may affect the current condition and alter the treatment plan.
- Medications used: Especially blood thinners (aspirin, warfarin, etc.) may increase bleeding risk and affect the treatment approach.
Physical Examination
- External Examination: I always begin the examination with inspection (visual examination). The shape of the nose, symmetry, swelling, bruising, and open wounds are carefully evaluated. Then, by gently palpating the nasal bones and lateral walls, I check for crepitation (crackling) or abnormal mobility. During this process, I also observe the patient’s pain response.
- Intranasal Examination: I evaluate the inside of the nose with anterior rhinoscopy or endoscopic examination. This examination is critical for checking septum position, mucosal condition, bleeding sources, and especially the presence of septal hematoma. During the examination, I reassure the patient by saying, “Now I will examine the inside of your nose, you may feel some discomfort but it will not be painful.”
- Evaluation of Surrounding Structures: Eye movements, facial bones, and dental occlusion are checked to investigate associated injuries. Particularly, the presence of double vision, limitation in eye movements, or problems with jaw closure are assessed. These findings may indicate a more extensive facial trauma rather than an isolated nasal fracture.
Imaging Methods
- Plain Radiography: It is usually sufficient for diagnosing simple nasal fractures. Lateral and Waters (semi-oblique) views are the projections we use most frequently. However, it may be insufficient in demonstrating small fractures or cartilage damage. In one of our patients, a fracture not visible on plain radiography but with persistent complaints was detected only by CT.
- Computed Tomography (CT): It is the method we prefer in complex fractures, cases where surrounding bone structures are affected, or for surgical planning. It shows bone structures in detail and allows 3D reconstruction. It is indispensable for preoperative planning, especially in naso-orbital or naso-ethmoidal complex fractures.
- Ultrasonography: It can be used especially in children to reduce radiation exposure. Its ability to show cartilage structures is an advantage. In our clinic, we primarily prefer ultrasonography in children under 10 years old. This method is advantageous both because it does not involve radiation and because it can be applied even if the child moves.
Diagnostic Challenges
Certain situations may create difficulties in diagnosing nasal fractures, and it is important to be aware of these challenges frequently encountered in clinical practice:
- Masking of deformity due to severe edema: Swelling that develops immediately after trauma may conceal the underlying deformity. Therefore, in suspicious cases, we re-evaluate after 5–7 days.
- Presence of old fracture or congenital deformity: The patient’s previous photographs or the nasal structure of family members may help in differential diagnosis.
- Small, non-displaced fractures: These fractures, which do not create noticeable deformity, may present only with tenderness and pain.
- Isolated septal fractures: The nose may appear normal externally, but there may be a fracture only in the septum. This condition can be detected through breathing difficulty and intranasal examination.
For this reason, in suspicious cases, I recommend re-evaluation after 5–7 days once the edema has subsided. During this period, we apply supportive treatments such as ice application (4–6 times a day for 15–20 minutes), head elevation (using 2–3 pillows while lying down), and pain control (such as paracetamol).
Once the diagnosis is established, the type of fracture, degree of displacement, associated injuries, and the patient’s general condition are taken into consideration for treatment planning. Early and accurate diagnosis is critical for selecting appropriate treatment and preventing complications. As I always tell my patients, “Proper treatment begins with proper diagnosis.”
Necessity of Surgical Treatment: When Surgery, When Conservative Treatment?
The decision-making process in the treatment of nasal fractures depends on the type of fracture, the patient’s symptoms, and aesthetic expectations. A question I frequently encounter in clinical practice is: “Doctor, do I need surgery?” The answer to this question is different for each patient, because not every nasal fracture requires surgery; many cases can be successfully treated with conservative methods.
Indications for Conservative Treatment
- Non-displaced Fractures: If the nasal bones are fractured but have maintained their normal position, surgery is usually not necessary. In this case, supportive treatment is sufficient. For example, in a young patient who sustained a mild blow while playing football and was found to have a fine crack on radiography, we achieved complete recovery with only rest and ice application.
- Minimal Deformity: Mild shape irregularities can be followed conservatively, especially if they do not bother the patient. In patients who say, “There is a slight curvature in my nose but it does not affect my breathing and I am not bothered by its appearance,” I do not recommend surgery.
- Isolated Soft Tissue Injuries: Surgery is not required in cases where only soft tissues are affected and there is no bone fracture. Although these patients may have bruising and swelling, these resolve spontaneously over time.
- Patient Preference: Some patients may accept minimal deformity and not want surgery. In the absence of medical indication, the patient’s preference may be decisive. A teacher patient once asked, “I don’t want to have surgery in the middle of the term, can we wait until summer break?” Since there was no functional problem, it was important to respect this preference and plan accordingly.
The conservative treatment approach includes:
- Pain control: Analgesics such as paracetamol are usually sufficient. NSAIDs (such as ibuprofen) are not recommended in the first 48 hours as they may increase bleeding risk.
- Edema-reducing measures: Ice application 4–6 times a day for 15–20 minutes and head elevation are effective in controlling edema.
- Nasal protection: Avoiding trauma, not wearing glasses, and not blowing the nose during the first weeks are recommended.
- Regular follow-up: Follow-up examinations are performed after 5–7 days when edema subsides and after 2–3 weeks when the fracture begins to heal.
Indications for Surgical Treatment
Marked Deformity: In the presence of visible curvature, collapse, or asymmetry of the nose, surgical correction is required. As in the case of a patient who said, “I don’t want to see my crooked nose every time I look in the mirror,” aesthetic concerns play an important role in the decision for surgery.
Functional Impairment: Septal deviation or narrowing of the nasal passage causing breathing difficulty is an indication for surgery. A patient who was an athlete presented with the complaint, “I can now only breathe through one nostril and it affects my performance.” In this case, surgical intervention was inevitable.
Septal Hematoma: Requires urgent drainage; otherwise, cartilage necrosis and nasal collapse (saddle nose deformity) may develop. In every patient in whom we detect a septal hematoma, we perform drainage immediately, even in the office setting.
Open Fractures: Surgical debridement and repair are required to reduce the risk of infection. In fractures with open skin wounds, cleaning and proper closure of the wound both reduce infection risk and improve aesthetic outcome.
Associated Injuries: Complex injuries such as naso-orbital or naso-ethmoidal fractures require surgery. In such complex fractures, a multidisciplinary approach may be necessary due to involvement of surrounding structures (orbit, sinuses, skull base).
Surgical Timing
The timing of surgical intervention is critical, and I pay special attention to this issue in my clinical practice:
Emergency Surgery (First 24 hours):
- Septal hematoma: Immediate drainage is required to prevent cartilage necrosis.
- Open fractures: Early intervention is necessary to reduce infection risk.
- Severe epistaxis (nosebleed): Surgical intervention may be required in uncontrolled bleeding.
- CSF leakage: CSF leakage due to skull base fracture requires urgent repair.
Early Surgery (3–10 days):
- Ideal period for closed reduction: During this period, edema has subsided but bone healing has not yet begun. It is the most appropriate time for closed reduction (external manipulation of fractured bones).
- In a boxing coach patient, we performed closed reduction 5 days after trauma. This timing was ideal both to wait for edema to subside and to intervene before the bones began to fuse.
Late Surgery (After 2–3 weeks):
- More invasive techniques may be required as bone healing has begun: Simple closed reduction is usually insufficient at this stage.
- Septoplasty or rhinoplasty may be considered: More comprehensive surgical interventions can be planned.
- In a patient who presented 1 month after trauma with noticeable nasal curvature, we had to use an open technique (rhinoplasty) instead of closed reduction.
Factors Affecting Treatment Decision
In my clinical practice, I always consider the following factors when making a treatment decision:
- Patient’s age: Growth potential should be considered in children. Especially in children under 14 years of age, more conservative approaches are preferred to avoid damaging the growth centers of the nasal bone and cartilage.
- General health status and comorbidities: Conditions such as diabetes and heart disease may increase surgical risk.
- Occupation and lifestyle: Functional and aesthetic outcomes may be more critical in professions such as professional athletes, musicians (especially wind instrument players), or actors.
- Aesthetic expectations: The patient’s expectations must be realistic and achievable. A patient who says, “I want my nose to look as if it was never broken after surgery,” should be gently informed that this may not always be possible.
- Previous nasal surgeries: Previous nasal surgeries may create technical challenges due to scar tissue and altered anatomy.
Preoperative Preparation and Expectations
Once the decision for nasal fracture surgery is made, the preoperative preparation process is of great importance for a successful outcome. This process includes preparing the patient physically and psychologically for surgery. In our clinic, we apply a personalized preparation protocol for each patient.
Preoperative Evaluation
Medical Evaluation:
- Detailed medical history: The patient’s past illnesses, surgeries, allergies, and medications are questioned. In one patient, unexpected bleeding occurred during surgery due to unreported aspirin use. Therefore, thoroughly questioning medication history is of vital importance.
- Physical examination: General health status, vital signs, and especially detailed examination of the nose and surrounding structures are performed.
- Anesthesia evaluation: This evaluation performed by the anesthesiologist is important for determining anesthesia risks and selecting the most appropriate anesthesia method.
- Required blood tests: Complete blood count, coagulation tests, and other biochemical tests if necessary are requested.
- ECG: Applied routinely especially in patients over 40 years old, depending on age and risk factors.
- Chest X-ray: Requested if necessary, especially in smokers or those with a history of lung disease.
Medication Adjustment:
- Aspirin and anticoagulants: These medications are discontinued 7–10 days before surgery. In one of our cardiac patients, we had to safely adjust anticoagulant therapy in consultation with the cardiologist.
- Vitamin E and herbal supplements: Should be discontinued at least 2 weeks before surgery as they may increase bleeding risk.
- Chronic disease medications: Medications for chronic diseases such as diabetes and hypertension are adjusted in consultation with relevant specialists.
Imaging and Planning:
- Current CT images: Especially in complex fractures, they guide surgical planning.
- Photographic documentation: Preoperative photographs taken from different angles are important for both planning and evaluating results.
- Explanation of the surgical plan to the patient: The technique to be used, expected results, and possible complications are explained in detail.
Patient Information
Before surgery, the patient is informed in detail about the following topics:
Surgical Process:
- Type of anesthesia: Simple closed reductions can usually be performed under local anesthesia, while more complex fractures or cases requiring septal repair may require general anesthesia.
- Duration of surgery: A simple closed reduction takes 15–20 minutes, whereas open techniques may take 1–2 hours. I provide clear information such as, “Your surgery will take approximately 45 minutes, but including preparation and recovery time, you should allocate 2–3 hours.”
- Technique to be used: Details such as whether closed reduction or open technique will be used and whether septal repair is necessary are explained.
- Expected results: To create realistic expectations, I make honest explanations such as, “We may not be able to restore your nose completely to its previous state, but we will achieve significant improvement.”
Risks and Complications:
- Bleeding: The most common complication, usually controlled with tampon placement.
- Infection: Rare, risk reduced with antibiotic prophylaxis.
- Anesthesia risks: General anesthesia has its own specific risks, which are explained by the anesthesiologist.
- Insufficient correction or asymmetry: Perfect results cannot be guaranteed in every surgery; minimal asymmetry may remain.
- Possibility of revision surgery: In some cases, a second surgery may be necessary.
Postoperative Process:
- Hospital stay: Usually a day-case procedure, but in some cases, a 1-night hospital stay may be required.
- Pain and edema expectations: I provide concrete information such as, “After surgery, there will be swelling and bruising around your nose and eyes for 2–3 days, but these will largely subside within 7–10 days.”
- Activity restrictions: The duration of avoiding activities such as sports, heavy lifting, and bending is explained.
- Healing process: Information is given about when tampons will be removed, how long a cast or splint will remain if applied, and follow-up appointments.
Day of Surgery Preparations
Preoperative Instructions:
- Fasting after midnight: If general anesthesia will be administered, fasting for at least 8 hours is recommended to reduce the risk of aspiration.
- Shower and hygiene: The patient is asked to shower on the morning of surgery and not to use makeup, creams, or similar products around the nose.
- Wearing comfortable clothing: Front-buttoned or zippered clothes that do not need to be pulled over the head should be preferred.
- No jewelry or makeup: Metal jewelry and makeup should be left at home as they will be removed during surgery.
- Arranging a companion: Especially if general anesthesia is administered, a companion is required to take the patient home.
Psychological Preparation:
- Creating realistic expectations: It is important to emphasize the message, “Surgery is not a miracle, healing will take time and the result will not be seen immediately.”
- Addressing concerns: I take time to patiently answer patients’ questions and alleviate their fears.
- Planning postoperative support: It is stated that assistance may be needed especially during the first days.
Special Situations
- Pediatric Patients: The principle of minimal intervention is applied considering growth potential in children. Family information and age-appropriate explanation to the child are important. I explained to the family of a 10-year-old patient, “Your child’s nose is still in the growth phase, so we will avoid very aggressive interventions.”
- Elderly Patients: Comorbidities, medications used, and anesthesia risks are evaluated in more detail. In a 75-year-old patient with hypertension, we had to change the anesthesia plan after cardiology consultation.
- Athletes: The recovery process and return-to-sport timing are specially planned. I informed a professional football player patient, “After surgery, you will need to stay away from contact sports for at least 4 weeks; include this period in your planning.”
The preoperative preparation process ensures not only physical readiness but also that the patient is psychologically prepared for surgery and the postoperative period. During this process, patient-physician communication and trust form the foundation for successful treatment. As I always tell my patients, “A good result begins with good preparation.”
Surgical Procedure: Step-by-Step Nasal Fracture Surgery
Nasal fracture surgery can be performed with different techniques depending on the type and complexity of the fracture. In my clinical practice, the methods I most frequently use are closed reduction and open reduction techniques. Both methods have their own specific indications and application steps. Now, I will explain this process step by step as it takes place in the operating room.
Closed Reduction Technique
Closed reduction is a minimally invasive technique that I prefer in simple nasal fractures and does not require skin incisions. It is usually performed within 3–10 days after trauma, once the edema has subsided.
Administration of Anesthesia:
The procedure can be performed under local anesthesia or mild sedation. First, I place cotton tampons soaked in 4% lidocaine and adrenaline inside the nose. These tampons are left in place for 10–15 minutes to ensure mucosal numbness. I also inject 2% lidocaine into the nasal dorsum and lateral walls. At each step, I reassure the patient by explaining what I am about to do, saying things like, “Now I will place an anesthetic medication inside your nose; you may feel a slight burning sensation, but it will pass quickly.”
Reduction Procedure:
- Special elevators are inserted into the nose: I place instruments such as Asch or Walsham forceps into the nose to support the fractured bones.
- Controlled pressure is applied externally with the fingers: While holding the instrument inside with one hand, I gently manipulate from the outside with the other hand.
- Fracture fragments are gently brought back to their normal positions: During this, I inform the patient, “You will feel slight pressure now; there should be no pain.”
- A “click” sound may be heard during the procedure: This sound indicates that the fracture fragments have settled into place and is a positive sign.
- Symmetry and smoothness are checked: During the procedure, I frequently assess the symmetry of the nose by looking from above and from the front.
Stabilization:
- Tampons are placed inside the nose: I usually use gauze soaked with antibiotic ointment or special nasal tampons. These tampons both control bleeding and support the reduced bones.
- A thermoplastic splint or plaster cast is applied externally: A splint made of special material that can be shaped when heated is placed over the nose and hardens after cooling, forming a protective shell.
- The splint is kept for 7–10 days: I explain to the patient, “This splint will ensure that the fractured bones remain in the correct position while healing, just like putting a cast on a broken arm.”
Open Reduction Technique
In complex fractures, when septal reconstruction is required, or when closed reduction fails, I prefer the open technique. Although this method is more invasive, it provides better results in correcting complex deformities.
Surgical Approach:
- Performed under general anesthesia: After the patient is put to sleep, an endotracheal tube is placed, and throat packing is applied to prevent blood aspiration.
- Incisions are made inside or outside the nose: In the endonasal approach, incisions are made inside the nose, while in the open rhinoplasty technique, a small incision is made on the columella (the tissue between the nostrils). This incision becomes almost invisible once healed.
- Fracture fragments are corrected under direct vision: After elevating the skin and soft tissues, the fractured bones are directly visualized and manipulated. This allows for more precise correction.
- If necessary, fixation with mini plates and screws is performed: In comminuted or unstable fractures, titanium mini plates and screws may be used to stabilize the bones. These materials can remain permanently in the body.
- If septal deviation is present, it is corrected in the same session: If curvature of the nasal septum causes breathing problems, it is corrected using septoplasty techniques.
Addition of Septoplasty:
If there is septal fracture or deviation:
- Mucoperichondrial flaps are elevated: The mucosal membrane covering the septal cartilage is carefully lifted without damaging the cartilage.
- Deviated cartilage and bone are removed or corrected: Curved cartilage fragments may be removed, reshaped, or straightened.
- The septum is fixed in the midline: The corrected septum is stabilized in the midline using special sutures or splints.
In one of my patients, there was both a nasal bone fracture and severe septal deviation. Using the open technique, I corrected the bones and performed septoplasty to resolve the breathing problem. When the patient came for follow-up 3 months later, he expressed satisfaction by saying, “I no longer snore at night and I wake up feeling more rested in the mornings.”
Intraoperative Evaluation
During surgery, I perform continuous checks:
- Evaluation of nasal symmetry: I check symmetry by looking from different angles.
- Assessment of airway patency: Especially in septal interventions, I ensure balanced airflow through both nostrils.
- Bleeding control: Bleeding sites are carefully checked during and at the end of surgery and stopped with electrocautery if necessary.
- Protection of adjacent structures: I take care to protect sensitive structures such as the eye area, sinuses, and skull base.
Special Situations and Additional Procedures
Septal Hematoma Drainage:
- Incision over the hematoma: A 0.5–1 cm incision is made on the mucosa.
- Removal of clots: Accumulated blood and clots are aspirated or cleaned with a small curette.
- Placement of a drain: A small drain may be placed to allow drainage if re-bleeding occurs.
- Tight packing: Both nostrils are tightly packed to bring the septal layers together.
In a boxer who presented to the emergency department, I detected a septal hematoma. I immediately performed drainage under local anesthesia and placed packing to prevent cartilage necrosis. I explained to the patient, “If we had not performed this intervention, the middle of your nose could have collapsed and permanent deformity could have developed.”
Naso-Orbital Fractures:
- Ophthalmology consultation: Eye movements, double vision, and intraocular pressure are evaluated.
- Orbital wall reconstruction: If there is a fracture in the orbital walls, it is repaired using special implants or grafts.
- Evaluation of the lacrimal system: Tear ducts are checked and repaired if necessary.
Pediatric Cases:
- Principle of minimal intervention: In children, the least invasive techniques possible are preferred to avoid damaging growth centers.
- Preservation of growth centers: Especially the growth centers at the nasal root must be protected.
- Use of absorbable materials: In children, dissolvable sutures and fixation materials are preferred.
In a 12-year-old patient with a nasal fracture due to a fall, I used a very gentle manipulation and a minimally invasive approach to preserve growth potential. I explained to the family, “Your child’s nose is still in the development stage, so we avoided very aggressive interventions.”
Recovery Process and Postoperative Care
The postoperative period is as important as the surgery itself. Proper care and follow-up prevent complications and ensure optimal healing. As I always tell my patients, “Half of the surgery is in the surgeon’s hands, the other half is completed with your care.”
First 24–48 Hours
Hospital Follow-up:
- Monitoring of vital signs: Blood pressure, pulse, and oxygen saturation are regularly checked. High blood pressure may increase bleeding risk.
- Bleeding control: The condition of the tampons and the amount of bleeding are frequently checked. I instruct the patient, “Slight oozing from the tampons is normal, but if there is continuous and active bleeding, inform us immediately.”
- Pain management: Mild analgesics such as paracetamol are usually sufficient. Severe pain is unexpected and should be reported to the physician.
- Head elevation: Keeping the head elevated at 30–45 degrees while lying down reduces edema and bleeding. I advise patients, “Keep your head elevated using two pillows; this will reduce swelling.”
Early Period Care:
- Ice application: During the first 48 hours, applying ice at 20-minute intervals is very effective in controlling edema. However, ice should be applied wrapped in a thin towel, not directly on the skin.
- Initiation of oral antibiotics: Antibiotic therapy is usually administered for 5–7 days to reduce infection risk.
- Analgesic therapy: Regular use of analgesics is recommended for pain control. Medications such as aspirin that increase bleeding risk should be avoided.
- Intranasal moisturizing sprays: Saline sprays may be used to prevent drying of the nasal mucosa.
First Week
Days 3–5:
- Intranasal tampons are removed: This procedure may cause mild discomfort but is not painful. I explain to the patient, “You will feel a slight pulling sensation while removing the tampons, but it will be very brief.”
- Mild bleeding is considered normal: After tampon removal, slight bleeding may occur for a few hours. In this case, it is recommended not to bend the head forward and to apply a cold compress to the nasal dorsum.
- Nasal irrigation can be started: After tampon removal, gentle irrigation with saline can be initiated to keep the inside of the nose clean.
Days 7–10:
- External splint is removed: The cast or splint on the nose is usually removed on days 7–10. At this stage, the patient can see the new shape of the nose for the first time, but it is not the final result due to remaining edema.
- Edema and bruising begin to subside: Bruising around the eyes usually turns yellow-green, indicating healing.
- Light activities are allowed: Light exercises such as walking can be started, but activities such as running and jumping should be avoided.
One of my patients became anxious after splint removal upon seeing that the nose was still swollen. I reassured them by saying, “This is a normal process; it may take 3–4 weeks for the edema to completely resolve, be patient.”
Between 2–4 Weeks
Activity Adjustment:
- Avoiding heavy physical activities: Activities that increase pulse and blood pressure may increase the risk of bleeding and edema. I advise patients, “Avoid heavy sports and exercises for 4 weeks.”
- Protection from nasal trauma: Be cautious in crowded environments and avoid contact sports.
- Care with glasses use: Since regular glasses put pressure on the nose, they should be temporarily supported with light taping or contact lenses should be preferred.
Follow-up Examinations:
- 2nd week control: The condition of edema, nasal shape, and function are evaluated.
- Endoscopic evaluation: Checked for intranasal adhesions or septal deviation.
- Photographic documentation: Photos are taken to monitor the healing process.
Long-Term Recovery
1–3 Months:
- Complete resolution of edema: Swelling over the nose usually completely subsides within 1–3 months. The nasal tip is the last area where edema decreases.
- Clarification of nasal shape: As edema decreases, the true shape of the nose becomes apparent.
- Return to normal activities: Most activities can be resumed after 6 weeks, and all activities including contact sports after 3 months.
6–12 Months:
- Evaluation of final result: The true result of surgery can only be fully evaluated after 6–12 months.
- Determination of need for revision: If there are aspects not satisfactory with the result, revision surgery can be planned at this stage.
One of my patients, when coming for follow-up 8 months after surgery, expressed satisfaction by saying, “At first I was worried that the swelling at the tip of my nose would not go away, but as you said, it completely resolved over time.”
Postoperative Recommendations
Things to Do:
- Regular use of prescribed medications: Antibiotics should be used until the course is completed.
- Intranasal cleaning and moisturizing: The inside of the nose should be regularly moisturized with saline sprays.
- Compliance with follow-up appointments: Regular check-ups are necessary to monitor the healing process.
- Protection from the sun: For the first 3 months, sun exposure may cause scars to darken; therefore sunscreen should be used or a hat worn.
Things to Avoid:
- Nose wiping: During the first 2 weeks, the nose should be wiped gently and blowing should be avoided. I instruct patients, “When wiping your nose, do so gently without pressing.”
- Hot showers and sauna: During the first week, hot showers, saunas, and steam baths may increase bleeding risk.
- Aspirin and alcohol: Aspirin and alcohol consumption that increase bleeding risk should be avoided during the first 2 weeks.
- Contact sports: Activities that carry a risk of nasal trauma should be avoided for 6–8 weeks.
Warning Signs
If the following situations develop, a doctor should be consulted immediately:
- Uncontrolled bleeding: Active nosebleed that cannot be stopped with pressure
- Severe increase in pain: Increasing pain not responding to analgesics
- Fever (above 38°C): May indicate infection
- Vision problems: Double vision, blurred vision, or limitation in eye movements
- Clear nasal discharge: May indicate CSF leakage
One of my patients presented urgently 5 days after surgery with a fever of 38.5°C and increasing nasal pain. Infection was detected on examination, and intravenous antibiotic therapy was initiated after hospital admission. Thanks to early intervention, recovery was achieved without developing a serious complication.
The recovery process may vary from person to person. Age, general health status, smoking, and the complexity of the surgery affect the speed of recovery. As I always tell my patients, “Being patient and following your doctor’s recommendations are the most important factors for a successful outcome.” Proper care and follow-up after nasal fracture surgery are the keys to achieving satisfactory results both functionally and aesthetically.
Potential Risks, Complications, and Limitations
Although nasal fracture surgery is generally a safe procedure, like any surgical intervention, it carries certain risks and complications. In my clinical practice, I observe that it is important for patients to understand these risks and develop realistic expectations for treatment success. As I always tell my patients, “Knowledge conquers fear” – therefore, openly sharing possible complications both strengthens the trust relationship and enables the patient to actively participate in the process.
Early Complications
- Bleeding: Mild bleeding during the first 24–48 hours after surgery is normal. However, severe or uncontrollable bleeding may suggest vascular injury and require intervention. In one patient, I had to take them back to the operating room due to bleeding that began 6 hours after surgery and did not stop despite packing. We stopped the bleeding by cauterizing the bleeding vessel with electrocautery. Although such situations are rare, it is always necessary to be prepared.
- Infection: Although rare, the risk increases especially in open fractures or immunocompromised patients. Antibiotic prophylaxis minimizes this risk. Signs of infection include increasing pain, redness, swelling, and fever. In a diabetic patient, we had to hospitalize them and administer intravenous antibiotics due to a postoperative infection.
- Hematoma: Accumulation of blood in the septum or soft tissues may require additional drainage. Septal hematoma is particularly important because, if not treated in time, it may lead to cartilage necrosis and “saddle nose” deformity. Therefore, I always evaluate the septum during early postoperative controls.
- Anesthesia Complications: Allergic reactions to local anesthesia or risks related to general anesthesia may occur. Detailed pre-anesthesia evaluation and history taking reduce these risks. In one patient, a mild reaction developed due to a previously undetected local anesthetic allergy. Therefore, thoroughly questioning anesthesia history is of vital importance.
Late Complications
- Insufficient Correction: Failure to fully correct the fracture may lead to residual deformity. This is especially seen in late-presenting or complex fractures. One of our patients presented 3 weeks after trauma, and since the bones had partially begun to fuse, we could not achieve full correction. Therefore, I emphasize the importance of early intervention.
- Overcorrection: Rarely, excessive intervention may result in unwanted shape changes. For example, if excessive correction is performed during lateral osteotomy (fracturing and narrowing the nasal side walls), the nose may become too narrow and a “pinched nose” appearance may occur.
- Septal Deviation: Septal problems not noticed during surgery or developing later may affect breathing. In one patient, we had to perform septoplasty 6 months later due to re-deviation of the septum after closed reduction.
- Sinusitis: Intranasal edema and anatomical changes may impair sinus drainage and lead to chronic sinusitis. This risk is higher especially in patients with previous sinus problems. I recommend nasal irrigation and moisturizing in the postoperative period for such patients.
- Olfactory Dysfunction: Although rare, permanent or temporary loss of smell may develop, especially in fractures affecting the upper nasal region. If the region where the smell receptors are located (olfactory cleft) is damaged, the sense of smell may be affected. In one patient, loss of smell that developed after severe trauma partially improved within 6 months.
Aesthetic Complications
- Asymmetry: Failure to achieve complete symmetry is the most common aesthetic issue. It is important to remember that perfect symmetry does not naturally exist in the human face. I always explain to my patients, “Perfect symmetry does not exist in nature; our goal is to achieve acceptable symmetry.”
- Nasal Dorsum Irregularities: Collapse, hump formation, or irregularities may be seen. Especially in comminuted fractures, it may be difficult to fully correct all fragments. In one patient, we later corrected a small irregularity remaining on the nasal dorsum with filler injection.
- Nasal Tip Problems: Particularly in cases with cartilage damage, nasal tip position may be affected. Drooping, asymmetry, or excessive rotation of the nasal tip may occur. These conditions can generally be corrected with a more comprehensive rhinoplasty.
- Skin and Soft Tissue Issues: Scar formation, subcutaneous irregularities, or thickening may occur. Especially when using an open technique, a small scar may remain on the columella. However, this scar usually fades over time and becomes almost invisible.
Functional Complications
- Chronic Nasal Obstruction: Permanent breathing difficulty may develop due to structural problems or mucosal edema. In one professional athlete patient, we had to perform additional septoplasty and turbinate reduction due to persistent breathing difficulty after surgery.
- Nasal Valve Insufficiency: Weakening of the nasal side walls may lead to collapse during inspiration and difficulty breathing. This condition becomes more pronounced during deep inhalation and is referred to as “nasal valve collapse.” Its treatment usually requires reinforcement with cartilage grafts.
Limitations of Treatment
- Anatomical Limitations: Severe cartilage loss or multiple previous traumas may prevent achieving ideal results. In one boxer patient, it was not possible to fully correct the complex deformity caused by repeated trauma. In such cases, presenting realistic expectations to the patient is very important.
- Healing Capacity: Factors such as age, smoking, and diabetes negatively affect healing. Especially in smokers, tissue oxygenation is reduced, so healing is slower and complication risk is higher. I recommend that these patients refrain from smoking for at least 2 weeks before and at least 4 weeks after surgery.
- Technical Limitations: Some complex deformities may not be fully corrected in a single session. Especially in complex fractures resulting from severe trauma, a staged surgical approach may be required. In one patient with a naso-orbital-ethmoidal complex fracture after a traffic accident, we performed emergency stabilization first and reconstructive surgery 6 months later.
Expected Results and Treatment Success
The expected results from nasal fracture surgery vary depending on the type of fracture, timing of treatment, and surgical technique. Creating realistic expectations is critical for patient satisfaction. I always explain to my patients, “Our goal is not perfection, but to achieve optimal results.”
Functional Results
- Improvement in Breathing: With appropriate treatment, breathing function returns to normal in 80–90% of patients. This rate is higher in cases where septoplasty is added. A marathon runner patient expressed satisfaction 2 months after surgery by saying, “I can now breathe through my nose, and this has positively affected my performance.”
- Sense of Smell: In most patients, the sense of smell is preserved or returns during the postoperative period. However, in severe trauma, especially if accompanied by skull base fracture, there is a risk of permanent olfactory dysfunction. This condition may significantly affect quality of life.
Aesthetic Results
- Shape Correction: In simple fractures treated early, satisfactory aesthetic results are achieved in up to 90% of cases. A model patient expressed satisfaction 3 months after surgery by saying, “No one can tell that my nose was broken; it looks very natural.”
- Natural Appearance: Modern surgical techniques ensure the preservation or reconstruction of natural nasal contours. The goal is not a “surgical look,” but to achieve a natural nose compatible with the patient’s facial structure. I always tell my patients, “A good nose surgery is one where no one can tell you had surgery.”
Factors Affecting Success
- Timing of surgery: Early intervention (within the first 2 weeks after trauma) yields better results. Interventions performed after the bones begin to fuse may produce less satisfactory outcomes.
- Complexity of the fracture: Results are better in simple, single-fragment fractures. It is more difficult to achieve full correction in comminuted, complex fractures.
- Surgeon’s experience: An experienced surgeon in nasal fracture treatment achieves better functional and aesthetic results. Therefore, especially in complex cases, choosing an experienced surgeon is important.
- Patient’s healing capacity: Healing is faster and complication risk is lower in young, healthy, non-smoking patients.
- Compliance with postoperative care: Results are better in patients who follow recommendations and attend regular follow-ups. One of our patients followed all recommendations meticulously and showed almost complete recovery within 3 weeks.
Patient Satisfaction
Based on my clinical experience, I can say that 85–95% patient satisfaction is achieved in surgeries performed with appropriate patient selection and technique. Reasons for dissatisfaction usually include:
- Unrealistic expectations: Expectations such as “It will return completely to its former state” or “There will be no scar at all” are generally not achievable.
- Residual deformity: Especially in complex fractures, full correction may not be achieved.
- Functional problems: Issues such as breathing difficulty or olfactory dysfunction may persist.
One of our patients said during the preoperative consultation, “I want my nose to be like it used to be.” I explained, “Our goal is to bring your nose as close as possible to its previous state, but we cannot guarantee exactly the same appearance as before the trauma.” Thanks to this realistic approach, although a small asymmetry remained after surgery, the patient was satisfied with the result.
Long-Term Follow-up and Care
Long-term follow-up after surgery is important for maintaining optimal results and early detection of late complications. I always emphasize the importance of follow-up by telling my patients, “Surgery is not an end, but a beginning.”
Regular Check-ups
First Year: Follow-up examinations are recommended at 1, 3, 6, and 12 months. During these check-ups:
- Functional evaluation: Functions such as breathing and sense of smell are tested.
- Monitoring aesthetic results: Nasal shape, symmetry, and healing are evaluated.
- Screening for complications: Possible late complications are investigated.
One of our patients described mild breathing difficulty at the 6-month follow-up. Endoscopic examination revealed a small adhesion (synechia) inside the nose, which was corrected with a simple intervention. This example demonstrates the importance of regular follow-up.
Long-Term: Annual check-ups or evaluation when symptoms develop are recommended. Especially in patients who have had a nasal fracture due to trauma, septal deviation or nasal valve problems may develop in later years. Therefore, evaluation is important when complaints arise.
Revision Surgery
According to my clinical experience, the need for revision is reported between 5–15%. Indications for revision include:
- Persistent deformity: Ongoing shape irregularity after surgery
- Functional problems: Persistent breathing difficulty
- Patient dissatisfaction: Dissatisfaction with aesthetic outcome
Revision surgery should be planned no earlier than 6–12 months. This period is necessary for complete tissue healing and resolution of edema. In one patient, we performed revision 9 months after the first surgery for a small irregularity on the nasal dorsum. The patient was very satisfied with the result after the second surgery.
Quality of Life
After successful treatment, patients:
- Can return to normal daily activities: Work, school, and social life are not affected.
- Can continue sports and physical activities: All activities can be resumed after an appropriate healing period.
- May experience increased self-confidence: Psychological improvement is observed especially in patients whose noticeable deformity has been corrected.
- Report improvement in breathing quality: Quality of life significantly increases in patients whose functional problems have been corrected.
An opera singer patient expressed satisfaction 3 months after surgery by saying, “I can breathe more comfortably now, and this has positively affected my performance. Also, I no longer need to make extra effort to conceal the curvature in my nose during stage makeup.”
Protective Measures
After treatment, nasal protection is important:
- Use of protective equipment in contact sports: Nasal protectors should be used in sports such as boxing and rugby.
- Avoiding trauma: Especially during the first 6 months, nasal trauma should be carefully avoided.
- Regular follow-up: Early evaluation is important if any complaints develop.
I recommended to one of my footballer patients to avoid contact sports for 3 months after surgery and to use a special nasal protective mask afterward. Thanks to these precautions, he was able to return to sports safely.
In conclusion, nasal fracture surgery is a treatment with a high success rate when applied with appropriate indication and technique. However, patients should be informed about potential risks and limitations, and realistic expectations should be established. Proper postoperative care and follow-up are critical for maintaining successful outcomes. As I always tell my patients, “A successful result is the product of cooperation between the surgeon and the patient.”

Prof. Dr. Murat Songu – Burun Estetiği (Rinoplasti) Uzmanı
Prof. Dr. Murat Songu, 1976 yılında İzmir’de doğmuş, tıp eğitimini Ege Üniversitesi Tıp Fakültesi’nde tamamladıktan sonra Celal Bayar Üniversitesi Kulak Burun Boğaz Anabilim Dalı’nda uzmanlık eğitimini tamamlamıştır. 2005–2006 yıllarında Fransa’nın Bordeaux kentinde Prof. Vincent Darrouzet ve Dr. Guy Lacher gibi rinoloji alanının önde gelen cerrahlarıyla çalışarak rinoplasti, fonksiyonel burun cerrahisi ve kafa tabanı cerrahisi üzerine ileri eğitim almıştır.
Burun estetiğinde doğal görünüm, nefes fonksiyonunun korunması ve yüz estetiği dengesini ön planda tutan Prof. Dr. Songu, açık teknik rinoplasti, piezo (ultrasonik) rinoplasti, revizyon rinoplasti, burun ucu estetiği ve fonksiyonel septorinoplasti operasyonlarında ulusal ve uluslararası düzeyde tanınan bir cerrahtır. Yurt içi ve yurt dışında çok sayıda rinoplasti kongresinde eğitici ve konuşmacı olarak yer almış; yüz estetiği ve burun cerrahisinde modern tekniklerin yaygınlaşmasına öncülük etmiştir.
100’den fazla bilimsel yayını, kitap bölümü yazarlıkları ve 1700’ü aşkın uluslararası atfıyla rinoplasti alanında Türkiye’nin en saygın akademisyenlerinden biri olan Prof. Dr. Murat Songu, doğal, yüzle uyumlu ve fonksiyonel sonuçlar hedefleyen cerrahi yaklaşımıyla hem bilimsel hem estetik başarıları bir araya getirmektedir.