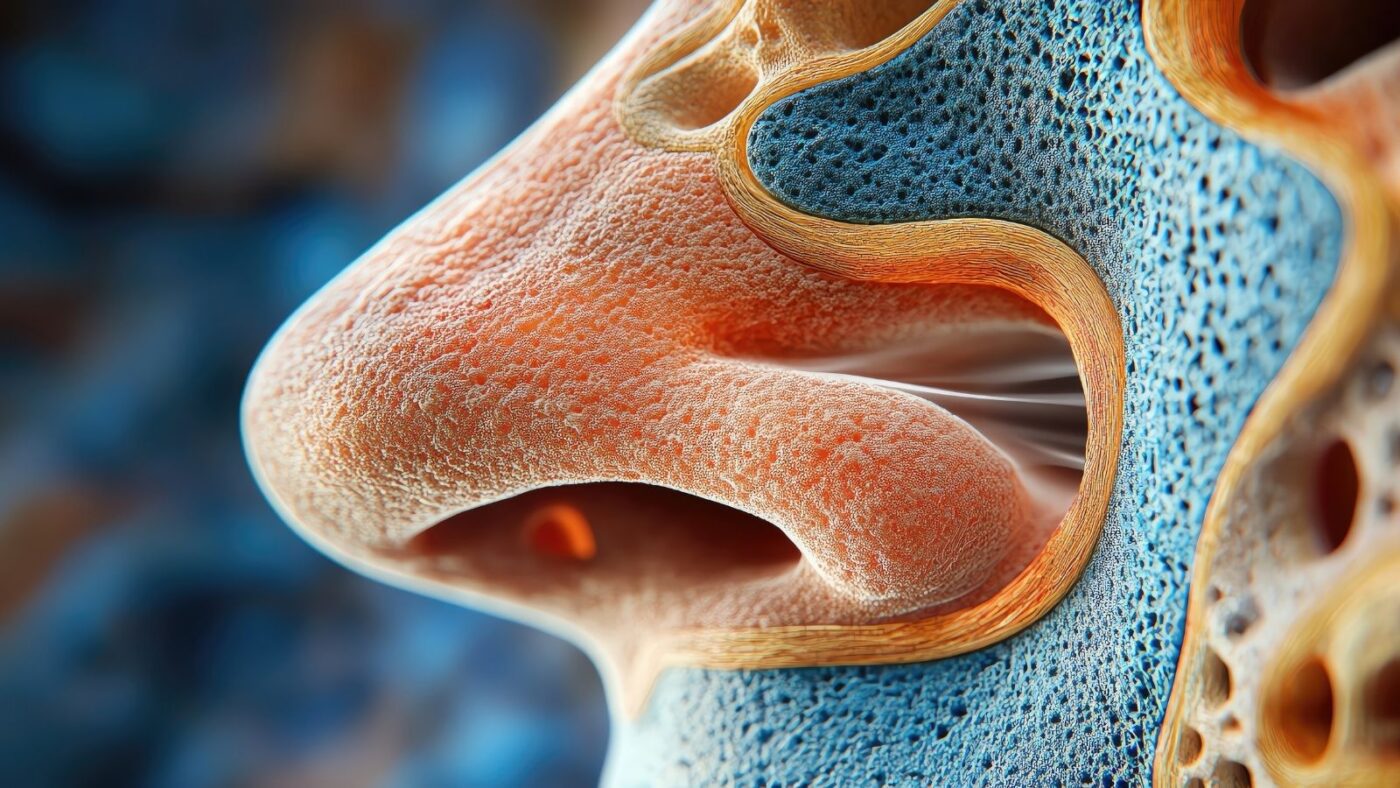
The upper lateral cartilage are special cartilage structures located on the side parts of our joints and are of vital importance for joint health. In medical terminology, the word “lateral” means “side” and describes areas that are away from the midline of the body. These cartilages are the silent heroes that make possible the movements we are not even aware of in daily life.
One of the most prominent examples of lateral cartilage in our body is the lateral meniscus in the knee joint. This C-shaped cartilage structure is located on the outer side of your knee and is engaged every time you take a step, climb stairs, or squat. Similarly, there are lateral cartilage structures in your ankle, shoulder, and hip. These structures are part of a complex system that ensures the proper functioning of the joints.
İçindekiler
Structure and Characteristics of Lateral Cartilage
Cartilage tissue is a special connective tissue that is neither as hard as bone nor as soft as muscle. It has a consistency somewhere between a biscuit and a sponge — firm enough to maintain its shape, yet capable of slight deformation under pressure and then returning to its original form. This feature allows lateral cartilages to function as perfect “shock absorbers” in the joints.
When examined under a microscope, we see that lateral cartilage tissue consists of three main components: cartilage cells called chondrocytes, collagen fibers, and proteoglycans. Chondrocytes are like the “workers” of the cartilage; they produce structural proteins and maintain the tissue. Collagen fibers are strong threads that provide resistance against tensile forces. Proteoglycans are large molecules that attract and retain water molecules — thus, when cartilage is compressed, it releases water, and when the pressure is removed, it reabsorbs water and returns to its original form.
Upper lateral cartilages may consist of different cartilage types such as hyaline cartilage and fibrocartilage. For example, while the lateral meniscus in the knee has a fibrocartilage structure, the lateral cartilages covering joint surfaces are generally hyaline cartilage. This difference is shaped according to the mechanical requirements of their location.
The Role of Lateral Cartilage in Joint Mechanics
When our joints move, friction occurs between the bones. If the bones were to come into direct contact, every movement would be painful and our bones would wear out quickly — just like an engine running without oil. Lateral cartilages minimize this friction and ensure smooth joint movement. The cartilage surface is so slippery that its coefficient of friction is even lower than that of a skate sliding on ice!
Another critical function of upper lateral cartilages is load distribution. For example, while walking, a load equal to 3-4 times your body weight is placed on your knee. Thanks to the lateral and medial menisci, this load is distributed over a wider area. Thus, the pressure on the surfaces of the bones that come into contact with each other decreases. You can think of this as the difference between narrow high-heeled shoes and wide-soled sneakers — when the same weight is distributed over a wider area, less pressure is applied to each point.
Upper lateral cartilages are also excellent shock absorbers. By absorbing the impacts that occur while running or jumping, they prevent these shocks from being directly transmitted to the bones and other joint structures. This feature protects our joints, especially during sports activities. With every jump of a basketball player or every step of a runner, the lateral cartilages quietly perform their duty.
Nutrition and Metabolism of Lateral Cartilage
Perhaps the most surprising feature of cartilage tissue is that it does not contain direct blood vessels. Almost all tissues in our body are nourished by blood vessels, but cartilage is an exception to this rule. So how is it nourished without blood vessels? The answer: diffusion.
Upper lateral cartilages obtain their nutrition through diffusion from the surrounding synovial fluid. Synovial fluid is a clear, egg-white–like fluid that fills the joint cavity. This fluid carries nutrients and oxygen. Cartilage cells absorb these nutrients like a sponge to survive. This is why joint movements are very important for cartilage health — as you move, synovial fluid is “pumped,” and the nutrition of the cartilage improves. In an immobile joint, cartilage cannot be adequately nourished and weakens over time.
This special mode of nutrition also affects the healing capacity of cartilage. Since it has no blood vessels, the healing process is very slow when injured, and complete healing often does not occur. Therefore, cartilage injuries are among the most challenging issues in orthopedic surgery. While small damages may heal on their own, large damages usually require surgical intervention.
Changes Seen in Upper Lateral Cartilage with Age
Like other tissues in our body, lateral cartilages undergo changes over time. These changes usually begin after the age of 30 and gradually progress. As we age, the water content of cartilage tissue decreases, its elasticity declines, and it becomes more fragile. This is similar to an old rubber band losing its flexibility.
These age-related changes are a normal process and a physiological change experienced by everyone. However, the speed and severity of these changes vary from person to person. Genetic factors, lifestyle, dietary habits, and previous injuries can affect this process.
It is important to understand the difference between normal aging and pathological changes. Mild thinning and loss of elasticity in cartilage with age are normal. However, complete wear of the cartilage, irregularities on the joint surface, and the development of bone spurs (osteophytes) are indicators of pathological processes such as osteoarthritis (calcification). In this case, unlike simple aging, symptoms such as joint pain, swelling, and limitation of movement occur.
Types of Upper Lateral Cartilage in Different Joints
In different joints of our body, there are lateral cartilage structures shaped according to the specific needs of that joint. These structures have developed special adaptations according to the movement pattern and load-bearing characteristics of the joint in which they are located. Just like different tools designed for different tasks, each lateral cartilage is “designed” appropriately for its own function.
The lateral meniscus in the knee is one of the best-known lateral cartilage structures. This C-shaped structure is located on the outer side of the knee joint and acts as a cushion between the femur (thigh bone) and tibia (shin bone). The lateral meniscus is more mobile than the medial (inner) meniscus and, thanks to this feature, can move more when the knee bends. This mobility protects it somewhat against injuries; therefore, lateral meniscus injuries are seen less frequently than medial meniscus injuries.
In the shoulder joint, lateral cartilage structures show a slightly different arrangement. The shoulder is the most mobile joint in our body and has a special design to provide this mobility. Here, the hyaline cartilage covering the joint surface between the head of the humerus (arm bone) and the scapula (shoulder blade) is slightly thicker in the lateral region. In addition, a fibrocartilage ring called the labrum deepens the joint socket and contributes to stability.
There is a similar arrangement in the hip joint. The hip joint is a ball-and-socket joint, and here too a fibrocartilage ring called the labrum surrounds the edge of the acetabulum (socket). While contributing to joint stabilization, this structure also plays a role in load distribution.
Other joints such as the ankle, wrist, and spine also have their own unique lateral cartilage structures. Each has evolved in accordance with the specific biomechanics of that joint.
Structural Differences of Upper Lateral Cartilages
Cartilage tissue is not uniform — there are three main types of cartilage in our body: hyaline cartilage, fibrocartilage, and elastic cartilage. Cartilages located in the lateral position also reflect this diversity.
Hyaline cartilage is the most common type of cartilage covering joint surfaces. It is smooth like glass and bluish-white in color. It contains a high amount of water and thus functions as an excellent shock absorber. The cartilages covering lateral joint surfaces are generally of this type. For example, the cartilage covering the lateral parts of the femur and tibia in the knee joint is hyaline type.
Fibrocartilage is a type of cartilage that contains more collagen fibers and is therefore more durable. It has high resistance to tensile forces. Structures such as the lateral meniscus in the knee and the labrum in the shoulder and hip are made of fibrocartilage. These structures provide stabilization in the joints and assist in load distribution.
Elastic cartilage, as its name suggests, contains elastic fibers and is therefore more flexible. It is found in structures such as the auricle of the ear and the Eustachian tube but is rarely encountered in joints.
Upper lateral cartilages differ in thickness, density, and elasticity depending on their location. For example, cartilages in regions that bear more load are generally thicker. In the knee joint, the cartilage in the lateral femoral condyle (outer side) is slightly thinner than the cartilage in the medial condyle (inner side) because it bears less load during walking.
Normal Anatomical Variations
Just as there are differences among people in height, weight, and eye color, normal variations are also seen in the structure of lateral cartilage. These differences are generally related to a person’s genetic structure, lifestyle, and level of physical activity.
For example, in some individuals, the lateral meniscus may have an abnormal shape called “discoid.” Instead of the normal C shape, it is more like a complete disk. This condition is usually congenital and often does not cause symptoms. However, it may sometimes lead to complaints such as catching or locking in the knee.
Gender, age, and ethnic origin may also affect the structure of lateral cartilage. Women generally have thinner cartilage structures than men. With age, cartilage thickness decreases and elasticity declines. In some ethnic groups, certain cartilage variations may be seen more frequently.
Athletes, especially professional athletes, may show adaptive changes in their lateral cartilage due to repetitive loading. For example, in long-distance runners, the cartilage in the knee joint may become more durable over time.
Pathological Changes and Deviations from Normal Structure
It is important to understand the difference between normal variations and pathological changes. Pathological changes usually lead to symptoms such as pain, limitation of movement, or impairment of joint function.
The most common pathological changes seen in upper lateral cartilage include degenerative changes (osteoarthritis), traumatic injuries, and inflammatory processes.
Degenerative changes are deterioration and thinning of cartilage tissue beyond normal age-related wear. This process is characterized by a decrease in the water content of cartilage, disorganization of collagen fibers, and a reduction in proteoglycan content. As a result, the cartilage surface becomes rough, and friction increases during joint movement. This leads to symptoms such as pain and stiffness.
Traumatic injuries are tears, cracks, or ruptures in cartilage resulting from a sudden blow or strain. For example, a lateral meniscus tear in the knee joint may occur as a result of sports injuries or sudden twisting movements. Such injuries may cause symptoms such as pain, swelling, a catching sensation, or locking in the joint.
Inflammatory processes are cartilage damages resulting from autoimmune diseases such as rheumatoid arthritis or infections. In this case, the body’s immune system mistakenly attacks its own cartilage tissue, or an infectious agent damages the cartilage. As a result, the cartilage structure deteriorates and pain, swelling, and limitation of movement occur in the joint.
Upper Lateral Cartilage Anomalies
In some cases, lateral cartilages may have a different structure from birth. While these anomalies sometimes cause no symptoms, they may sometimes lead to joint problems at an early age.
Among congenital lateral cartilage anomalies, the best known is the discoid lateral meniscus mentioned earlier. Instead of the normal C shape, this variation has a more complete disk shape and may affect the normal function of the meniscus. Although it often causes no symptoms, it may sometimes lead to complaints such as catching, locking, or pain in the knee.
Other congenital anomalies include genetic diseases that affect cartilage development. For example, a group of diseases called chondrodysplasias affect cartilage formation and development. These conditions usually manifest with symptoms such as short stature, joint deformities, and early-onset osteoarthritis.
Acquired lateral cartilage disorders are cartilage damages that occur after birth due to various reasons. Factors such as trauma, repetitive micro-traumas, infections, metabolic diseases, or medication use may lead to changes in cartilage structure. For example, long-term steroid use may cause weakening of cartilage tissue and make it more susceptible to damage.
Upper Lateral Cartilage Injuries and Trauma
Upper lateral cartilages may be damaged especially in sports injuries and accidents. A sudden blow, sprain, or excessive loading may cause these delicate structures to tear or fragment. Cartilage injuries may seriously affect joint function and, if left untreated, may lead to permanent damage.
Lateral meniscus injuries in the knee are among the most common lateral cartilage traumas. These injuries usually occur as a result of a sudden twisting movement while the knee is in a flexed position. They are common in sports such as football, basketball, and skiing. Since the lateral meniscus is more mobile than the medial meniscus, the risk of injury is slightly lower, but it is still a frequently encountered condition.
Patients often state that they heard a “pop” sound at the moment of injury or felt sudden pain in the joint. This may be a sign that the cartilage has torn. Subsequently, swelling, limitation of movement, and pain that increases with weight-bearing develop in the joint. In some patients, the knee may “lock” — this occurs when a torn meniscus fragment becomes trapped in the joint space and makes it impossible to fully straighten or bend the knee.
In addition to acute injuries, repetitive small traumas may also create an accumulation of damage in lateral cartilages over time. This is called “chronic microtrauma.” For example, in long-distance runners or people who work in jobs requiring constant squatting, microscopic cracks may form in the cartilage tissue as a result of repetitive loading. These cracks may merge over time and lead to larger damages. Patients usually feel gradually increasing pain and discomfort without a distinct injury.
Degenerative Upper Lateral Cartilage Diseases
Wear and tear in lateral cartilages with aging is normal. However, some factors may accelerate this process. Excess weight, repetitive trauma, genetic predisposition, and certain metabolic diseases accelerate the degenerative process. This accelerated degeneration is called osteoarthritis (calcification).
Osteoarthritis is characterized by the gradual thinning and eventual complete wear of cartilage tissue. This process also leads to changes in the bone beneath the cartilage — the bone hardens (subchondral sclerosis) and bone spurs (osteophytes) form at the edges. Upper lateral cartilage degeneration is especially common in the knee and hip joints.
The degenerative process usually progresses in four stages:
- Stage: Mild softening and swelling on the cartilage surface
- Stage: Cracks and fibrillation (rough appearance) on the cartilage surface
- Stage: Deep cracks and cartilage loss
- Stage: Complete wear of the cartilage and exposure of the underlying bone
While patients initially feel mild discomfort, the severity of pain increases over time. Morning stiffness, pain after activity, and cracking sounds in the joint are typical complaints. In advanced stages, joint deformity and significant limitation of movement may develop.
Measures that can be taken to reduce the risk of upper lateral cartilage degeneration include:
- Maintaining ideal weight (Every 1 kg of excess weight adds 3-4 kg of additional load to the knee joint while walking and 7-8 kg while climbing stairs)
- Regular, joint-friendly exercises (such as swimming, cycling)
- Avoiding joint trauma and properly treating injuries
- Balanced nutrition and adequate vitamin D intake
- Avoiding repetitive excessive loading
Inflammatory Processes and Upper Lateral Cartilage
Some systemic diseases cause the body to attack its own tissues. These autoimmune processes may also affect lateral cartilages. The inflamed joint lining secretes enzymes that erode cartilage and gradually deteriorate its structure.
Rheumatoid arthritis is the most common inflammatory disease affecting lateral cartilages. In this disease, the immune system mistakenly attacks the joint lining (synovium). The inflamed synovium thickens and forms a tissue called “pannus.” This tissue invades the cartilage and secretes enzymes that dissolve it. Rheumatoid arthritis usually affects the joints symmetrically — meaning the same joints on both sides are affected. Morning stiffness, joint swelling, and pain are typical symptoms. Stiffness lasting longer than one hour is a distinguishing feature compared to the short-term stiffness seen in osteoarthritis.
Crystal arthropathies are diseases caused by the accumulation of various crystals in the joints. In gout, uric acid crystals accumulate, while in pseudogout, calcium pyrophosphate crystals accumulate in the joint. These crystals cause damage on the lateral cartilage surface and lead to severe pain attacks.
In gout, the uric acid level in the body increases and this acid accumulates in the joints in crystal form. Although it most commonly affects the big toe joint, it may also be seen in the knee, ankle, and other joints. A gout attack usually begins suddenly at night; the affected joint becomes red, swollen, and extremely sensitive to touch. The attack usually resolves spontaneously within a few days but may recur.
Pseudogout (false gout) occurs due to the accumulation of calcium pyrophosphate crystals in the joints. It shows symptoms similar to gout but usually affects joints such as the knee, wrist, and elbow. It is more common in the elderly population.
Infectious arthritis (septic arthritis) is a serious condition that occurs when bacteria directly enter the joint. The bacteria may rapidly destroy cartilage and, if left untreated, may lead to permanent joint damage. Severe pain, swelling, redness, and fever in the affected joint are typical symptoms. This condition is a medical emergency and requires immediate antibiotic treatment.
Congenital Upper Lateral Cartilage Anomalies
Some babies are born with lateral cartilage anomalies. These conditions are usually noticed during routine examinations or when the child begins to walk. Congenital anomalies may occur as a result of genetic factors, environmental influences during pregnancy, or disruptions in the developmental process.
Congenital lateral cartilage malformations can be classified in various ways. Some appear as isolated anomalies, while others may be part of a broader syndrome. For example, the discoid lateral meniscus mentioned earlier is an isolated anomaly and usually does not cause a serious problem. However, in genetic diseases such as some chondrodysplasias, all cartilage tissues are affected and this may lead to serious skeletal deformities.
Developmental hip dysplasia is a condition characterized by insufficient development of the lateral acetabular cartilage (the socket part of the hip joint). If not diagnosed and treated early, this anomaly increases the risk of hip dislocation and early osteoarthritis in later life. Stability tests of the hip joint performed during newborn examinations can detect this condition at an early stage.
Metabolic diseases may also affect lateral cartilage development. For example, in lysosomal storage diseases such as mucopolysaccharidoses, abnormal substances accumulated in cells may disrupt cartilage development. This condition may lead to symptoms such as joint deformities, short stature, and limitation of movement.
Early diagnosis and treatment are critical for these children to achieve normal joint function. If families notice gait disturbances, leg length differences, or joint deformities in their children, they should definitely consult a specialist. Treatment varies according to the type and severity of the anomaly — in some cases physical therapy and special devices are sufficient, while in others surgical intervention may be required.
Upper Lateral Cartilage Tumors and Rare Conditions
Tumor development in upper lateral cartilages is rare but may occur. Although most are benign, some may be malignant and early diagnosis is of vital importance. Cartilage tumors originate from cartilage cells (chondrocytes) or from cells capable of forming cartilage.
Among benign cartilage tumors, the most common is enchondroma. This tumor is usually seen in the bones of the hands and feet but may rarely affect joint cartilages. It often causes no symptoms and is detected incidentally on an X-ray taken for another reason. Osteochondroma is a protrusion arising from the surface of the bone and covered with cartilage. It usually occurs near the growth plates of long bones and stops growing when growth is completed.
The most common malignant cartilage tumor is chondrosarcoma. This tumor originates from cartilage cells and is usually seen in the pelvis, ribs, shoulder, and long bones. It presents with pain, swelling, and sometimes a palpable mass. Treatment is usually surgical, and chemotherapy or radiotherapy may be added depending on the grade of the tumor.
Synovial chondromatosis is a rare condition characterized by the abnormal production of cartilage nodules by the joint lining (synovium). These nodules may break off over time and become loose bodies within the joint cavity. It most commonly affects the knee, hip, and elbow joints. It may cause symptoms such as joint pain, swelling, limitation of movement, and sometimes a locking sensation. Treatment is usually arthroscopic surgery to remove the loose bodies.
These rare conditions usually present with long-standing joint complaints that do not respond to treatment. Imaging methods play a critical role in diagnosis. MRI, CT, and sometimes biopsy may be required for a definitive diagnosis. Early diagnosis and appropriate treatment are very important for preserving joint function and increasing survival in malignant tumors.
Physical Examination Techniques in Upper Lateral Cartilage Evaluation
When a patient consults a doctor with suspicion of a lateral cartilage problem, the first step is a detailed physical examination. This examination is the cornerstone of the diagnostic process and provides valuable information before imaging methods. The doctor first observes the patient’s gait, examines the shape of the joint, and checks for swelling.
During the examination, the doctor moves the joint at various angles and evaluates whether pain occurs during these movements and whether there is limitation of movement. For example, when a lateral meniscus problem is suspected in the knee joint, special maneuvers such as the McMurray test are performed. In this test, the doctor bends the patient’s knee and then slowly extends it while rotating it to check whether the torn part of the meniscus becomes trapped in the joint space. If trapping occurs, the patient feels pain or a “click” sound may be heard.
The patient is asked to perform certain movements — such as squatting or simulating climbing stairs. The location and character of the pain during these movements provide important clues. In upper lateral cartilage problems, pain is usually localized on the side of the joint. The doctor also evaluates sensitive points around the joint by palpation (examining by hand).
During the physical examination, the stability of the joint is also checked. For example, in the knee joint, the integrity of the lateral collateral ligament is evaluated with the varus stress test. This test is important to detect ligament injuries that may accompany lateral cartilage injuries.
Examination findings are evaluated together with the patient’s complaints and medical history to determine possible diagnoses and decide on the necessary imaging methods.
Evaluation of Upper Lateral Cartilage with Imaging Methods
X-ray is usually the first requested imaging method. However, cartilage tissue is not visible on X-ray; only indirect findings such as narrowing of the joint space are evaluated. X-ray is excellent for showing bone structure and helps detect conditions such as fractures, dislocations, or advanced osteoarthritis. For the patient, X-ray imaging is quite simple — images are taken in different positions within a few minutes. It is a painless procedure and the radiation dose is low.
Magnetic Resonance Imaging (MRI) is the best method for visualizing lateral cartilages. It perfectly images soft tissues and shows the location, type, and degree of cartilage damage in detail. During MRI scanning, the patient enters a narrow tube and must remain still for approximately 20-40 minutes. The device makes loud noises while operating, so patients are given headphones. Some patients may experience fear of enclosed spaces (claustrophobia). In this case, open MRI devices may be preferred or a mild sedative may be given.
Special protocols are used for lateral cartilage evaluation in MRI. For example, in knee MRI, special sequences are added to better visualize the lateral meniscus. Cartilage damage appears as signal changes on MRI. In mild damages, only increased signal within the cartilage is seen, while in advanced damages, findings such as cartilage loss and bone marrow edema may be detected.
Ultrasound is particularly useful in the evaluation of superficial lateral cartilages. It is successful in showing cartilage structures close to the surface in joints such as the knee, ankle, and elbow. Ultrasound is a dynamic examination method — meaning the joint can also be evaluated while in motion. This provides an advantage especially in detecting irregularities on the cartilage surface or loose bodies. It is a completely painless procedure for the patient — the doctor obtains images by moving a gel-applied probe over the skin. During the procedure, the doctor may ask the patient to perform various movements.
Computed Tomography (CT) is not as successful as MRI in cartilage evaluation but may be preferred in some special cases. It is particularly superior in showing calcifications within cartilage or changes in bone structure. In a special technique called CT arthrography, contrast material is injected into the joint to examine the cartilage surface in more detail. This method is preferred especially in patients who cannot undergo MRI (such as patients with pacemakers) or in cases where MRI is insufficient.
When Should Medical Help Be Sought?
Patients should consult a specialist without delay in the following situations:
- Sudden onset of severe pain and swelling in the joint: This may be a sign of an acute cartilage injury or intra-articular bleeding. Especially severe pain and swelling developing after trauma require urgent evaluation.
- Inability to move the joint or bear weight: If the patient cannot move the joint or bear weight on the affected extremity, this may be a sign of a serious injury. For example, locking may occur as a result of a lateral meniscus tear in the knee joint and the patient cannot fully straighten the knee.
- Locking sensation in the joint: This condition occurs when a piece of cartilage becomes trapped in the joint space and prevents full movement of the joint. It usually requires surgical intervention.
- Joint pain accompanied by fever: This combination may be a sign of septic arthritis (joint infection) and requires urgent antibiotic treatment. If treatment is delayed, cartilage may be rapidly destroyed.
- Joint deformity after trauma: This may be a sign of fracture or dislocation and requires urgent intervention.
Slowly developing but progressively worsening complaints also require evaluation. Symptoms such as morning stiffness, pain increasing after activity, and cracking sounds in the joint suggest lateral cartilage problems. These symptoms may be harbingers of degenerative processes such as osteoarthritis. Early diagnosis and treatment may slow the progression of the disease and preserve joint function.
In addition, patients who have previously been diagnosed with a cartilage problem should consult a doctor if their symptoms suddenly worsen or new symptoms develop. This may mean progression of the disease or the development of a new complication.
Patient Experience in the Diagnostic Process
When the patient comes for the first examination, a detailed history is first taken. The doctor asks when the pain started, its character, and what increases or decreases it. Questions such as “Does your pain increase with movement or with rest?”, “Do you feel stiffness in the morning?”, “Have you experienced locking or giving way in the joint?” provide important clues in the diagnostic process. Previous traumas, family history of joint disease, and medications used are questioned.
The physical examination usually lasts 15-20 minutes. The doctor may ask the patient to remove clothing (for example, wearing shorts may be necessary for knee examination). Some movements may be painful, but the doctor informs the patient in advance: “I will now move your knee, please warn me if there is pain.” During the examination, the doctor evaluates the appearance of the joint, swelling, increase in temperature, range of motion, and stability. By applying special tests, the doctor tries to understand which structures are affected.
After the examination, the doctor shares the findings with the patient and requests the necessary imaging tests. Explanations such as “I suspect a meniscus tear, we need to have an MRI to confirm this” are made. Appointments are usually given for imaging tests. Metal objects must be removed for MRI, and patients with pacemakers cannot undergo MRI. The patient is informed that fasting is not required before the scan but that they must remain still.
Imaging results are usually available within a few days. In some centers, the patient receives the results on a CD and takes them to the doctor; in others, the results are transmitted electronically to the doctor. After all tests are completed, the doctor explains the findings to the patient in understandable language. By showing the images, the doctor points out the problem in the lateral cartilage: “Look, there is a tear in your meniscus here, that is why you are experiencing pain and locking.”
Treatment options are explained together with their risks and benefits. “We can start with conservative treatment — rest, ice application, anti-inflammatory medications, and physical therapy. If this approach is not sufficient, we may consider arthroscopic surgery.” The patient may ask for time to decide on the treatment plan or seek a second opinion. The doctor answers the patient’s questions and addresses concerns.
Advanced Diagnostic Methods
In some cases, imaging methods may not provide sufficient information. Arthroscopy is a minimally invasive method that can be used for both diagnostic and therapeutic purposes. By entering the joint through small incisions, the lateral cartilage is directly visualized. This procedure is usually performed in the operating room under local or general anesthesia.
During arthroscopy, a camera (arthroscope) with a diameter of 4-5 mm is placed inside the joint. This camera magnifies the interior of the joint and displays it on a monitor. The doctor can examine the cartilage surface in detail and evaluate the location and degree of damage. In the same session, treatment can also be performed if necessary — for example, a torn meniscus can be repaired or irreparable parts can be removed.
The patient can usually go home the same day. Pain and swelling may occur for a few days after the procedure, but these are usually controlled with ice application and painkillers. The patient is informed about when they can return to normal activities and about the rehabilitation program.
If a tumor is suspected, a tissue sample may need to be taken from the lateral cartilage. This procedure is performed under local anesthesia and with imaging guidance. A small piece of tissue is taken from the suspicious area with a thin needle and sent for pathological examination. The patient can go home the same day. Results are usually available within a few days.
Blood tests are especially important in the differential diagnosis of inflammatory diseases. Tests such as rheumatoid factor, anti-CCP, and uric acid level are requested. High CRP and sedimentation rate indicate the presence of an active inflammatory process. If gout is suspected, serum uric acid level is measured. However, during an acute gout attack, uric acid levels may be normal, so joint fluid analysis may be required for definitive diagnosis.
Joint fluid analysis involves taking fluid from the joint with a needle (arthrocentesis) and examining this fluid in the laboratory. The color, viscosity, cell count, and crystal analysis of the fluid are performed. If infection is suspected, the fluid is sent for culture. This analysis is very valuable in making a differential diagnosis between infectious arthritis, crystal arthropathies, and inflammatory arthritis.
Advanced diagnostic methods are critical for the correct diagnosis of lateral cartilage problems. Correct diagnosis forms the basis for creating an appropriate treatment plan and achieving the best outcome for the patient.
Conservative Treatment Approaches in Upper Lateral Cartilage Problems
In the treatment of upper lateral cartilage problems, non-surgical methods are generally the first choice. This approach is called “conservative treatment” and provides successful results in many patients. The main components of conservative treatment are: physical therapy and rehabilitation, medical treatment, intra-articular injections, and the use of supportive devices.
The physical therapy program is customized according to the patient’s condition. A physiotherapist designs an exercise program based on the patient’s age, physical condition, and type of cartilage problem. This program usually consists of three main components: flexibility exercises, strengthening exercises, and proprioception (balance and coordination) exercises. The patient attends physical therapy 2-3 times a week, for a total of 15-20 sessions. Each session lasts approximately 45-60 minutes.
Physical therapy sessions usually proceed as follows: First, light aerobic activity for warm-up (such as a stationary bike), followed by manual therapy (special maneuvers performed by the physiotherapist with their hands), then exercises, and finally a cool-down period. At the end of the session, ice application or electrotherapy (such as TENS, ultrasound) may be performed to reduce pain and inflammation. The physiotherapist also gives exercises to be done at home and teaches the correct technique.
Medical treatment is used to control pain and inflammation. Non-steroidal anti-inflammatory drugs (NSAIDs) are the most commonly used medications. Drugs such as ibuprofen, naproxen, and diclofenac both reduce pain and suppress inflammation. The doctor selects the appropriate medication by evaluating the patient’s stomach problems, kidney functions, and other medications used. In some patients, stomach-protective medications may also be prescribed. Regular use of medications and monitoring of side effects are important. The patient should immediately inform the doctor if symptoms such as stomach pain, indigestion, or black stools occur.
In cases of severe pain, stronger painkillers (such as tramadol) may be used for a short period. However, long-term use should be avoided due to their potential for dependence. In some patients, supplements such as glucosamine and chondroitin sulfate are recommended. These substances may help preserve and repair cartilage structure, but scientific data on their effectiveness are conflicting.
Intra-articular injections are another important component of conservative treatment. Corticosteroid injections provide rapid pain control but are recommended not to be administered more than 3-4 times a year. Because repeated injections may damage cartilage tissue. Before injection, the joint area is cleaned with an antiseptic solution and a local anesthetic spray may be applied. The procedure usually takes a few minutes and causes minimal pain. After the injection, the patient should rest the joint for 24-48 hours.
Hyaluronic acid injections (viscosupplementation) act as joint lubricants. Hyaluronic acid, the main component of natural joint fluid, is synthetically produced and injected into the joint. This treatment is usually administered once a week for 3-5 weeks. The duration of effect may be up to 6 months. The injection is performed under sterile conditions, usually with ultrasound guidance. The patient should rest the joint for 24 hours after the procedure.
In recent years, regenerative treatments such as platelet-rich plasma (PRP) and stem cell injections have also gained popularity. These treatments aim to activate the body’s own healing mechanisms. PRP is obtained from the patient’s own blood and is rich in growth factors. Stem cell treatments aim to promote cartilage regeneration. However, more scientific research is needed regarding the effectiveness of these treatments.
Orthoses and supportive devices are used to protect and stabilize the joint in lateral cartilage problems. For example, a knee brace may be recommended for a patient with a lateral meniscus injury in the knee joint. This brace limits excessive movement of the joint and improves load distribution. In ankle problems, special insoles or ankle braces may be used. These devices enable the patient to perform daily activities more comfortably and contribute to the healing process.
Surgical Treatment Options
Surgery is considered in patients who do not respond to conservative treatment. Surgical treatment is planned according to the type and location of cartilage damage and the patient’s age and activity level. Various options are available such as arthroscopic surgery, open surgery, cartilage transplantation, and prosthetic applications.
Arthroscopic lateral cartilage surgery is a minimally invasive method performed through small incisions. This technique offers less pain, faster recovery, and a lower risk of complications. Arthroscopy is especially ideal for meniscus tears, irregularities on the cartilage surface, and removal of loose bodies.
Before arthroscopic surgery, the patient usually fasts for 8 hours before the operation. The procedure is performed under general anesthesia or spinal anesthesia. The surgeon makes 2-3 small incisions (each approximately 0.5-1 cm) to access different areas of the joint. One of these incisions is used for the camera and the others for surgical instruments. During the procedure, the joint is filled with a special fluid — this improves visibility and provides bleeding control.
In case of a meniscus tear, the surgeon may perform repair or partial meniscectomy (removal of the damaged part) depending on the type and location of the tear. Irregularities on the cartilage surface are corrected with special instruments (debridement). Loose bodies are removed. The procedure usually takes 30-60 minutes. The patient is usually discharged the same day or the next day.
Open surgical methods may be required in larger and more complex lateral cartilage damages. In this case, a larger incision is made to directly visualize the joint. Open surgery is especially preferred in situations such as repair of large cartilage defects, complex meniscus transplantation, or ligament reconstruction.
The preparation process before open surgery includes blood tests, anesthesia evaluation, and cleaning of the surgical area. The patient is usually hospitalized one day before the surgery. The hospital stay after surgery may be 2-3 days. The recovery process is longer compared to arthroscopic surgery, and more pain and swelling may be observed.
Cartilage transplantation may be considered in young patients. Autologous chondrocyte implantation (ACI) is a procedure in which the patient’s own cartilage cells are multiplied in the laboratory and transplanted to the damaged area. This technique is especially effective in localized cartilage defects. The procedure is two-stage: In the first stage, a small piece of healthy cartilage is taken and the cells are multiplied in the laboratory. In the second stage, the multiplied cells are transplanted to the defective area. Full recovery may take 6-12 months, but the results are generally very good.
Mosaicplasty (osteochondral autograft transfer) is a procedure in which healthy cartilage-bone blocks are taken from less load-bearing areas of the joint and transplanted to the damaged area. This technique is especially effective in small and medium-sized defects. The procedure is completed in a single session and the recovery process is shorter.
In cases of advanced lateral cartilage damage where other treatment options have failed, prosthetic applications may be considered. Total joint prosthesis is the procedure of replacing the entire joint with an artificial joint. Partial (unicompartmental) prosthesis replaces only the damaged part of the joint. Prosthetic surgery is generally preferred in elderly patients and those with severe osteoarthritis. The hospital stay after surgery may be 3-5 days and full recovery may take 3-6 months.
Recovery Process and Expectations
With physical therapy and medical treatment, significant improvement is seen in most patients within 6-8 weeks. However, full recovery may take 3-6 months. During this period, patient compliance with treatment is critical. Regularly performing recommended exercises, using medications correctly, and adhering to activity restrictions directly affect treatment success.
During conservative treatment, the patient usually feels a reduction in pain within the first 1-2 weeks. Symptoms such as swelling and stiffness also decrease over time. Within 4-6 weeks, most patients become able to perform daily activities comfortably. However, full recovery and return to sports may take longer. The patient’s age, degree and type of cartilage damage, accompanying problems, and compliance with treatment are factors affecting the recovery time.
Post-surgical rehabilitation protocols vary according to the type of surgery performed. In general, ice application, elevation, and rest are recommended for the first 48 hours after surgery. This is important to control pain and swelling. The patient usually begins simple exercises immediately after surgery — for example, contracting the quadriceps muscle. This is necessary to prevent muscle atrophy and improve circulation.
Physical therapy usually begins in the first week. In the initial sessions, the goal is to increase range of motion and gain basic muscle strength. Over time, more advanced exercises are introduced. The time to full weight-bearing varies according to the type of surgery — it may be 2-4 weeks after arthroscopic procedures and 6-12 weeks after open surgery. During this period, the patient may use crutches or a cane.
During the rehabilitation process, the physiotherapist and doctor regularly evaluate the patient’s progress. Parameters such as pain, swelling, range of motion, and muscle strength are monitored. If necessary, the rehabilitation program is adjusted according to the patient’s condition. Active participation and motivation of the patient are very important for a successful outcome.
Return to daily activities usually occurs within 4-6 weeks. The patient becomes able to perform basic activities such as housework, going to work, and driving. However, strenuous activities such as heavy lifting or prolonged standing may need to be avoided for some time. Return to sports activities may take 3-6 months. The doctor allows activity after evaluating reduction in pain, restoration of range of motion, and adequacy of muscle strength.
Long-term prognosis depends on the type of cartilage damage, the patient’s age, and activity level. In young patients with small meniscus tears or superficial cartilage damage, full recovery and return to normal function are expected. However, in elderly patients with large cartilage defects or advanced osteoarthritis, certain activity limitations may persist. In patients who have undergone prosthetic surgery, the lifespan of the prosthesis is generally 15-20 years, after which revision surgery may be required.
Practical Recommendations for Patients
During the recovery process, the patient should take an active role. Exercises recommended by the doctor should be performed regularly 2-3 times a day. It is important to work within the pain limit without excessive strain. A mild feeling of discomfort during exercise may be normal, but if severe pain is felt, the exercise should be stopped. Exercises improve cartilage nutrition, increase muscle strength, and provide joint stability.
Simple measures that can be applied at home include:
- PRICE protocol: Protection, Rest, Ice, Compression, Elevation. It is effective in acute injuries and flare-up periods.
- Ice application: Apply an ice pack wrapped in a towel for 15-20 minutes, 3-4 times a day. This reduces pain and swelling.
- Elevation: The affected joint is kept above heart level. This helps reduce swelling.
- Compression: Elastic bandages or special compression stockings may be used. However, it should not be too tight.
- Proper posture and body mechanics: Simple precautions such as bending the knees when lifting heavy objects and avoiding staying in the same position for a long time protect the joints.
Weight control is critical for lateral cartilage health. Every extra kilogram places 3-4 times more load on the joints. For example, 5 kg of excess weight adds 15-20 kg of additional load to the knee joint while walking and 35-40 kg while climbing stairs. Therefore, reaching and maintaining ideal weight is one of the most important steps for cartilage health.
Nutrition also affects cartilage health. A diet rich in omega-3 (such as salmon, walnuts, flaxseed) may have anti-inflammatory effects. Fruits and vegetables rich in antioxidants, foods containing vitamin C (necessary for cartilage collagen synthesis), and adequate protein intake are recommended. Avoiding excessive sugar and processed foods may reduce inflammation. Adequate water consumption is also important for cartilage hydration.
Activity modifications are an important management strategy in lateral cartilage problems. Instead of high-impact sports (such as running, basketball, football), joint-friendly activities such as swimming, cycling, and using an elliptical trainer should be preferred. These activities place minimal load on the joints while being beneficial for cardiovascular health and muscle strength. Warm-up before activity and cool-down exercises afterward reduce the risk of injury.
Use of appropriate footwear, proper walking technique, and an ergonomic work environment protect lateral cartilages. Shoes should have a good shock-absorbing sole and support the foot. High-heeled shoes increase the load on the knee and hip joints and should be avoided. For those who work sitting for long periods, taking regular breaks and performing simple stretching exercises are recommended.
Regular follow-ups after treatment are important. The first follow-up is usually planned 2-4 weeks later, and subsequent follow-ups every 3-6 months. During these visits, the effectiveness of the treatment is evaluated and the plan is revised if necessary. Patients should consult a doctor without delay if increased pain, swelling, or limitation of movement develops.
Complications and Management
Every treatment has risks. In conservative treatment, stomach irritation, kidney function impairment, or allergic reactions may occur due to NSAID use. The risk of infection with injections is less than 0.1%, but caution should be exercised. Repeated corticosteroid injections may increase cartilage damage. Patients should understand these risks and immediately inform their doctor if any side effects develop.
After surgery, bleeding, infection, and stiffness may develop. The risk of complications in arthroscopic surgery is low (1-2%), but it is slightly higher in open surgery. Signs of infection (redness, swelling, increased temperature, discharge, fever) should be carefully monitored. The risk of deep vein thrombosis (DVT) increases especially in prolonged surgeries and immobilized patients. To reduce this risk, early mobilization and sometimes blood-thinning medications are used.
With early diagnosis and intervention, most complications can be successfully treated. In case of infection, antibiotic treatment and sometimes surgical debridement may be required. If stiffness develops, intensive physical therapy and sometimes manipulation (forcibly moving the joint under anesthesia) may be applied. If DVT is suspected, diagnosis is made with Doppler ultrasound and anticoagulant treatment is initiated.
If one treatment method fails, alternatives are evaluated. Surgery may be considered for a patient who does not respond to conservative treatment, and revision surgery may be considered for failed surgery. For example, if meniscus repair fails, partial meniscectomy; if cartilage transplantation fails, prosthetic surgery may be evaluated as alternatives. In every case, the most appropriate treatment is selected considering the patient’s age, activity level, and expectations.
Chronic pain may develop in some patients. In this case, a multidisciplinary approach is required. Pain clinics, psychological support, and alternative treatment methods may be evaluated. In chronic pain management, methods such as medications (antidepressants, anticonvulsants), physical therapy, TENS (Transcutaneous Electrical Nerve Stimulation), acupuncture, and cognitive behavioral therapy may be used. The patient should develop strategies to cope with pain and maintain an active lifestyle as much as possible.
Upper lateral cartilage problems can be successfully managed with correct diagnosis and appropriate treatment. The patient’s active participation in the treatment process, lifestyle changes, and regular follow-ups are critical for long-term success. An individualized approach for each patient is the key to achieving the best results.

Prof. Dr. Murat Songu – Burun Estetiği (Rinoplasti) Uzmanı
Prof. Dr. Murat Songu, 1976 yılında İzmir’de doğmuş, tıp eğitimini Ege Üniversitesi Tıp Fakültesi’nde tamamladıktan sonra Celal Bayar Üniversitesi Kulak Burun Boğaz Anabilim Dalı’nda uzmanlık eğitimini tamamlamıştır. 2005–2006 yıllarında Fransa’nın Bordeaux kentinde Prof. Vincent Darrouzet ve Dr. Guy Lacher gibi rinoloji alanının önde gelen cerrahlarıyla çalışarak rinoplasti, fonksiyonel burun cerrahisi ve kafa tabanı cerrahisi üzerine ileri eğitim almıştır.
Burun estetiğinde doğal görünüm, nefes fonksiyonunun korunması ve yüz estetiği dengesini ön planda tutan Prof. Dr. Songu, açık teknik rinoplasti, piezo (ultrasonik) rinoplasti, revizyon rinoplasti, burun ucu estetiği ve fonksiyonel septorinoplasti operasyonlarında ulusal ve uluslararası düzeyde tanınan bir cerrahtır. Yurt içi ve yurt dışında çok sayıda rinoplasti kongresinde eğitici ve konuşmacı olarak yer almış; yüz estetiği ve burun cerrahisinde modern tekniklerin yaygınlaşmasına öncülük etmiştir.
100’den fazla bilimsel yayını, kitap bölümü yazarlıkları ve 1700’ü aşkın uluslararası atfıyla rinoplasti alanında Türkiye’nin en saygın akademisyenlerinden biri olan Prof. Dr. Murat Songu, doğal, yüzle uyumlu ve fonksiyonel sonuçlar hedefleyen cerrahi yaklaşımıyla hem bilimsel hem estetik başarıları bir araya getirmektedir.